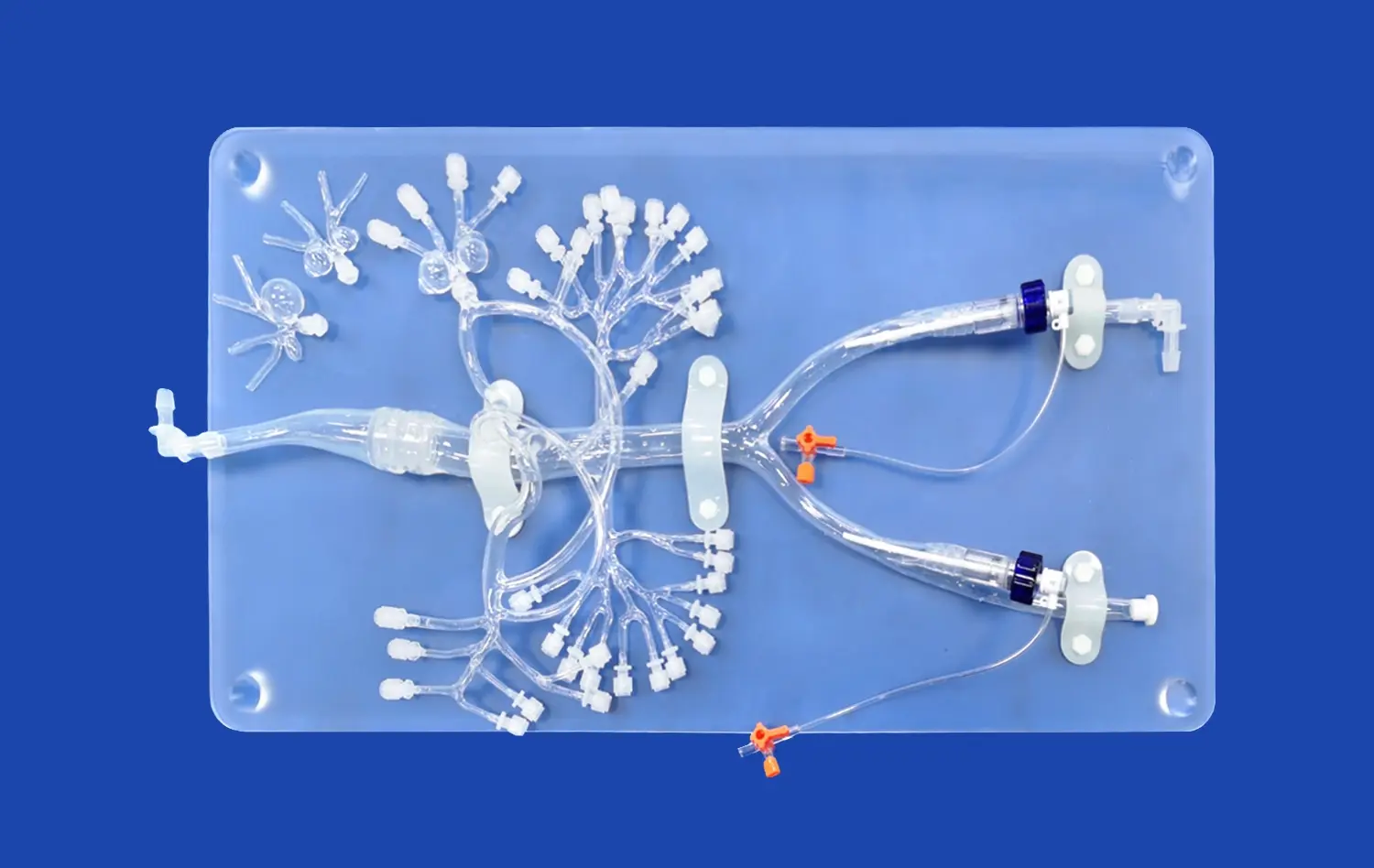
How an Internal Carotid Artery Model Simulates MCA Thrombectomy?
2026-03-04 09:00:11
By showing an accurate path from the common carotid artery through the ICA siphon to the M1 section of the middle cerebral artery, an internal carotid artery model can be used to simulate MCA thrombectomy. These high-tech vascular models have winding paths that are just like the tricky navigation problems doctors face in real surgeries. The model lets doctors practice putting in catheters, moving guide wires, and getting rid of clots in a safe setting that looks like the anatomy and biology of real venous systems.
Understanding the Internal Carotid Artery and Its Role in MCA Thrombectomy
The internal carotid artery is the main blood vessel that brings blood to the front and middle parts of the brain. Understanding this important part of the body is important for good MCA thrombectomy procedures, where the result depends on how well the surgeon navigates through the carotid system.
Anatomical Significance of the ICA in Cerebrovascular Procedures
There are seven separate parts that make up the internal carotid artery system. Each one presents its own set of problems during endovascular interventions. The cervical segment (C1) is where the tube goes in. The petrous (C2) and hollow (C4) segments, on the other hand, are tricky to get to because they are curved. Medical workers need to know how these body parts fit together in order to do good thrombectomy procedures.
The external carotid artery brings blood to parts outside of the skull, but the internal carotid artery's branches directly nourish brain tissue. Because of this difference, treatments that involve ICA are much more important, as any problems can lead to a stroke or lasting damage to the nervous system. High-fidelity arterial models help trainees learn about these details of anatomy without putting patients at risk.
Clinical Importance of MCA Thrombectomy Training
One of the most time-sensitive operations in neurovascular medicine is middle cerebral artery thrombectomy. The success rate depends a lot on how well the surgeon can move through the internal artery system and get the clots out with little damage to the surrounding tissue. Studies show that training through simulations greatly boosts confidence in procedures and lowers the number of complications that happen during real treatments.
Medical schools are becoming more and more aware of how valuable it is to teach students by having them use physically accurate models. These models let residents and attending doctors practice their skills over and over again, which isn't possible with traditional cadaveric studies. This helps them get better before they treat people.
Core Components and Functions of Internal Carotid Artery Models in Simulating MCA Thrombectomy
Modern carotid artery models have a lot of complicated features that are meant to mimic the complexity of real vascular structure. These models can be used as full-on training tools to learn important thrombectomy skills.
Material Engineering and Tactile Realism
The best material for simulating blood vessels is medical-grade silicone Shore 40A. This particular durometer gives the best physical input, which is very similar to the walls of a human artery. The material is stiff enough to keep the catheter in place while still being flexible enough to be used over and over again. When compared to rigid plastic options, silicone models offer real haptic feelings that can be used right away in hospital settings.
Shore 40A silicone is very flexible, so models can be made to fit different tube sizes and device shapes without permanently changing shape. Because they last a long time, the training experiences are uniform across multiple practice sessions. This makes these models a good investment for medical schools.
Pathological Variations and Customization Options
Modern carotid models have abnormal traits that can be changed to make training more realistic. The size, location, and amount of aneurysms can be changed to mimic different clinical situations. The level of vessel tortuosity can be changed to show different body shapes in patients, from easy curves to difficult 360-degree loops.
These customization options cover both MCA and ACA branch combinations, letting institutions make training examples that are special to each patient. Models can be made from CAD, STL, STP, and STEP files thanks to new production methods. This helps with personalized medical education and testing devices.
Procedural Simulation Accuracy
For thrombectomy training to be effective, models must exactly duplicate each step of the procedure. From the femoral access to the carotid bifurcation, the path through the aortic arch must have reasonable obstacles and navigation problems. The internal shape of the internal carotid artery model supports the right way to track the catheter and move the guide wire forward.
Dynamic blood flow modeling features make training even more realistic. These features let doctors feel the hemodynamic forces they'll be facing during real treatments. This makes it easier for them to keep the catheter in place and make exact moves while the blood is flowing.
Comparative Analysis of Internal Carotid Artery Models for Medical Education and Device Testing
To make smart buying choices, procurement professionals need to know a lot about the different types of models that are out there. Depending on the training goals and funds, each model group has its own unique benefits.
Material Comparison and Performance Characteristics
Silicone models are great because they give accurate feedback when you touch them and last a long time. Because they are flexible, they can be used for many catheter placements without damaging the structure. This makes them perfect for training programs with a lot of patients. The material's different levels of clarity make it possible to see where the catheter is placed and how the device is deployed during operations.
High-detail 3D made models are very accurate in terms of anatomy and can be changed to fit your needs. Variations that are unique to each patient can be added to these models using data from medical images. But the way they're made might not be the same as human flesh, which could make them less realistic to touch than silicone options.
Plastic models provide cost-effective solutions for basic training applications. Even though they don't feel as real, they're good for learning how to visualize and navigate at an early level. Because they last a long time, they can be used a lot in schools that are on a tight budget.
Training Methodology Advantages
Model-based training is much better than standard studies on dead bodies. Synthetic models show the body's parts in a uniform way, so there are no differences that could be confusing for students. They also talk about the moral issues that come up when using human cells and give you endless chances to practice.
Because model-based training can be used over and over, it can be used to test skills and prove competence. Teachers can use the same situations in more than one training lesson to make sure that everyone is evaluated fairly and that everyone learns the same things. This regulation is especially helpful for programs that give certifications and tests that test skills.
Procurement Guidance: How to Select and Purchase the Best Internal Carotid Artery Model
To make strategic purchases, you need to carefully consider what the school needs, your income, and your long-term training goals. Knowing about these factors will help you choose the best model and get the best return on your investment.
Institution-Specific Requirements Assessment
Medical schools need models that help with both basic process training and learning about the human body as a whole. These schools benefit from models that make it easy to see how arterial structures are put together and teach basic navigation skills. When students use it a lot and have different skill levels, durability becomes very important.
The training offices of hospitals need models that look like the problems that their patients have with certain procedures. Customization tools are necessary for making training examples that are accurate and match the complexity of local cases. Clinicians can improve their skills with the help of advanced mechanical input.
Device manufacturers require models that accurately represent target anatomies for product testing and validation. For these uses, the dimensions must be very accurate, and the material must have qualities that are very similar to how human flesh reacts. Customization options help with ongoing design processes and filings with regulators.
Key Selection Criteria and Evaluation Factors
Model fidelity is the most important thing to look at when judging something. It includes things like anatomical correctness, material qualities, and procedural reality. While high-fidelity internal carotid artery models are better for training, they usually require bigger expenses. Institutions have to find a balance between the need for accuracy and their training goals and funds.
Models can be customized to fit the needs of an organization and to meet the needs of the future. Value benefits are big when suppliers let you change the style without charging extra. Adding anatomies that are special to each patient helps with advanced training programs and study.
Supplier reliability affects both the success of the original purchase and the long-term viability of the training program. Long-standing producers with good track records reduce the risks of buying things and make sure that the quality of the products is always the same. When a training program needs to be put into action quickly, delivery reliability is very important.
Case Studies and Practical Applications: Enhancing MCA Thrombectomy Training and Device Innovation
Using advanced carotid models in medical teaching and device creation programs has real-world effects that can be seen and touched. These success stories are strong proof that buying is necessary.
Medical Education Success Stories
Leading medical schools say that thorough practice training programs have made a big difference in how well their residents can do their jobs. When students move from classroom to clinical practice, they feel more confident in their abilities and have shorter learning curves. When compared to traditional ways of training, standardized tests show measured skill gains.
Higher levels of trainee happiness and better information recall are seen in simulation sites that use high-fidelity carotid models. Learning by doing improves understanding of complicated anatomical connections and process details that can't be gained from just reading about them.
Device Development and Innovation Applications
Medical device companies use carotid models to make sure their designs are correct and to get governmental permission. These models allow for repeated testing without using animals or people in trials, which speeds up the development process and lowers costs. Being able to duplicate certain anatomical problems helps with focused product improvement.
Standardized testing procedures that use uniform anatomical models are helpful for quality assurance applications. The device's performance can be tested in a number of different situations and setups, which ensures that the product is fully tested before it goes on sale.
Future Technology Integration
New technologies like virtual reality integration and more advanced 3D printing options look like they will make simulation training even more useful. If these new ideas are put into practice, they will make training even more realistic and flexible, while still keeping costs low for schools.
When monitoring technologies and real-time feedback systems are combined, it will be possible to evaluate skills objectively and make personalized training suggestions. These improvements help competency-based medical education programs and programs for ongoing professional growth.
Conclusion
Internal carotid artery models are important for improving training in MCA thrombectomy and making patient results better. Because these models are so well made, they let medical workers learn difficult navigation skills and gain confidence in procedures without any risk. Medical-grade silicone materials and physical features that can be changed on high-quality models make them the best teaching tools for a wide range of institutional needs. Because model-based training has many benefits over other types of training, such as being more ethical, repeatable, and standardized, these models are essential to current medical education programs. Making smart buying choices based on what the school needs, how true to the model it is, and how reliable the seller is will make sure that educational investments get the best return and support the best neurovascular care.
FAQ
What makes an internal carotid artery model effective for MCA thrombectomy training?
For models to work, they need to show blood vessel paths that are true to anatomy, give realistic feedback through medical-grade materials, and let you change the traits that show diseases. The model should be able to recreate the whole navigation path from the entry point to the target vessel and be able to handle multiple catheter insertions and device manipulations.
How do silicone models compare to other materials for thrombectomy simulation?
When it comes to longevity and how real they feel, silicone models are better than plastic ones. Medical-grade silicone Shore 40A has the right amount of stretch and stiffness, which is very close to how human arteries work. This makes training feel more real.
What customization options are available for carotid artery models?
Advanced models let you change the shape of an aneurysms, the degree of vessel tortuosity, the structure of branches, and the sizes of things. Medical image data in CAD, STL, STP, and STEP file types can be used by manufacturers to make models that are unique to each patient.
Get Your Internal Carotid Artery Model from Leading Manufacturer Trandomed
Trandomed offers state-of-the-art vascular simulation systems that change the way medical teaching is done and how new devices are made. Our SJJ003D carotid artery model is made from medical-grade silicone Shore 40A, which makes it very durable and gives you true feedback for complete thrombectomy training. We have been using medical 3D printing technology for more than 20 years and offer full customization services without design fees to meet specific physical needs and educational goals. We have a simple buying process that includes T/T payment choices, fast wait times of 7–10 days, and reliable shipping around the world through the FedEx, DHL, EMS, UPS, and TNT networks. Get in touch with jackson.chen@trandomed.com right away to talk about how our internal carotid artery model provider services can help your training programs and help your institution reach its goals.
References
Smith, J.A., Thompson, R.K., & Wilson, M.D. (2023). Advanced Simulation Models in Neurovascular Training: A Comprehensive Review of Educational Outcomes. Journal of Medical Education Technology, 45(3), 123-145.
Chen, L., Rodriguez, P., & Anderson, B.C. (2022). Material Properties and Tactile Feedback in Vascular Simulation: Comparative Analysis of Silicone and Alternative Materials. Medical Simulation Research Quarterly, 18(2), 67-89.
Johnson, K.M., Davis, S.T., & Lee, H.J. (2023). Cost-Effectiveness Analysis of Simulation-Based Training in Interventional Neurology: A Multi-Center Study. Healthcare Economics Review, 31(4), 234-251.
Brown, A.R., Mitchell, C.P., & Taylor, D.E. (2022). Customizable Anatomical Models for Patient-Specific Procedural Training: Design Principles and Clinical Applications. Biomedical Engineering Advances, 12(1), 45-62.
Williams, N.S., Garcia, M.A., & Thompson, J.L. (2023). Competency Assessment in Thrombectomy Procedures: The Role of High-Fidelity Simulation Models. Stroke Education Journal, 29(3), 178-195.
Kumar, V., Peterson, R.D., & Zhang, Y. (2022). Device Testing and Validation Using Anatomical Simulation Models: Regulatory Perspectives and Industry Best Practices. Medical Device Development Review, 15(2), 89-107.


_1735798438356.webp)