Internal Carotid Artery Model for Catheter and Guidewire Navigation
2026-03-02 09:00:09
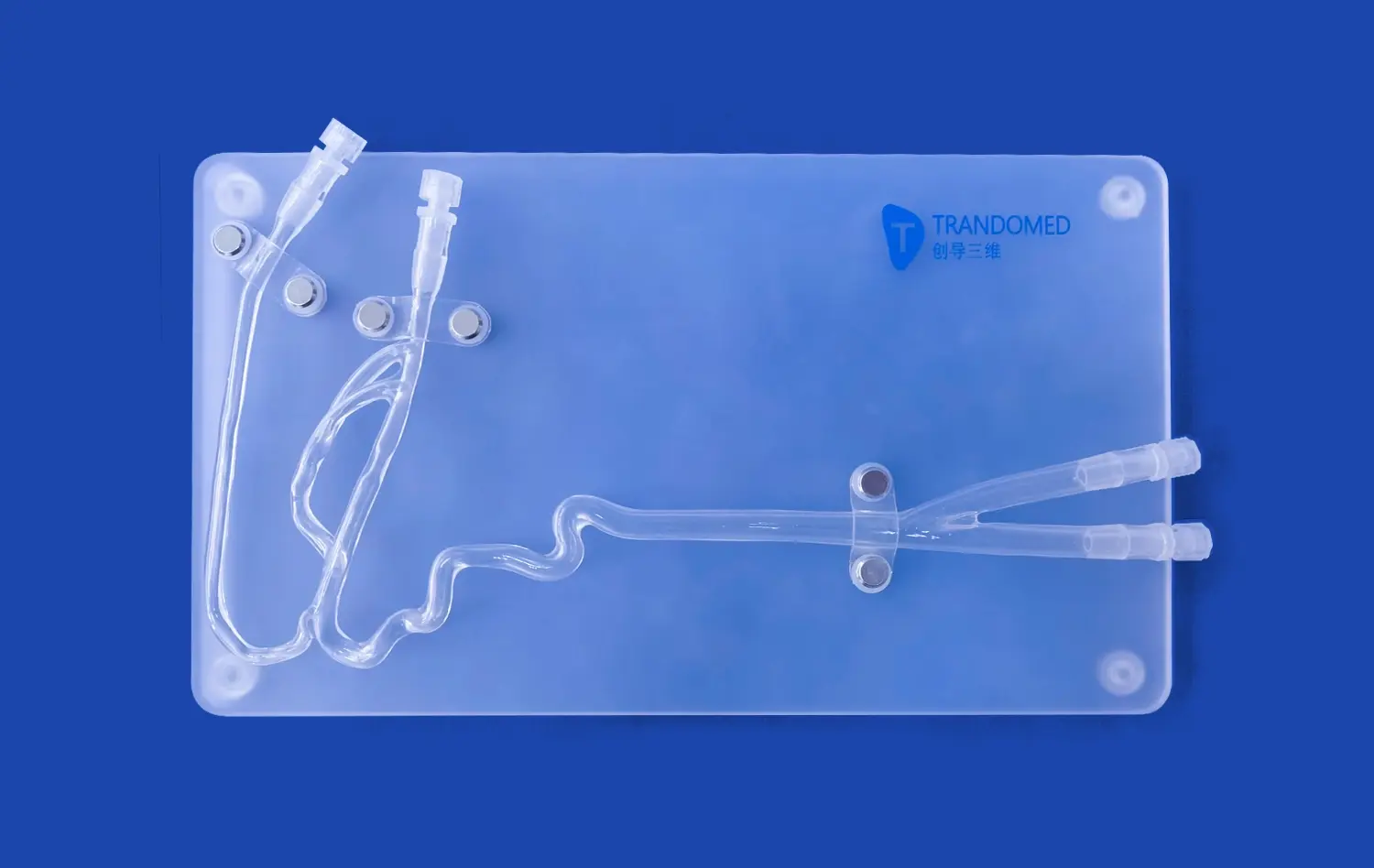
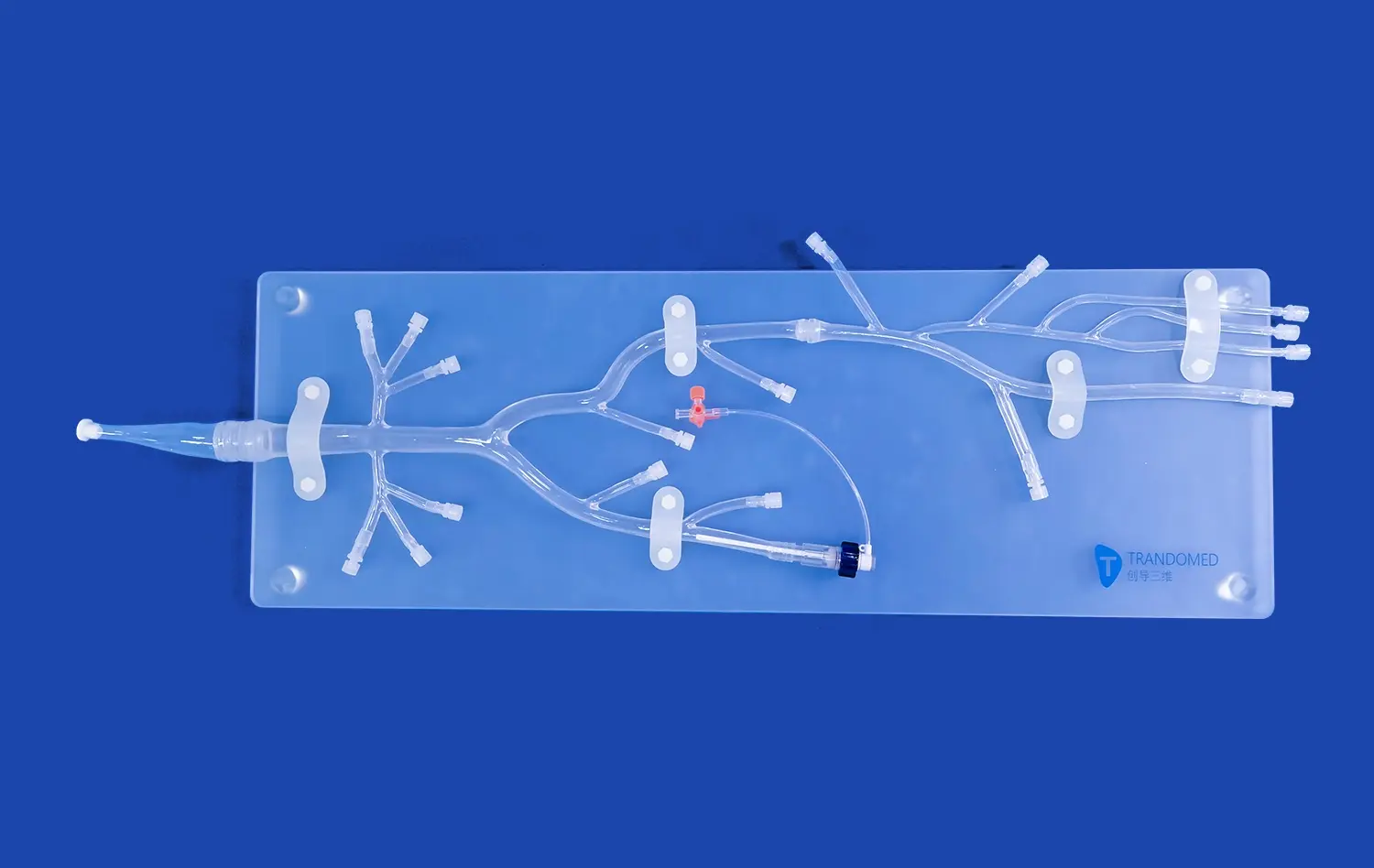
The internal carotid artery model represents a breakthrough in medical simulation technology, specifically designed to enhance catheter and guidewire navigation training for healthcare professionals. These sophisticated anatomical replicas provide realistic representations of the complex vascular pathways within the carotid system, enabling medical practitioners to develop essential skills in endovascular procedures. Modern simulation models incorporate detailed lumen structures, realistic tortuosity patterns, and pathological variations that mirror actual patient anatomy, making them indispensable tools for contemporary medical education and device development.
Understanding Internal Carotid Artery Models and Their Applications
Precision and reality are important in modern medical training that can't be taught in the same way in the past. This problem is fixed by internal carotid artery computer models, which show complicated vascular structure in a real, three-dimensional way. The complex design elements in these learning tools are meant to mimic the complicated paths that doctors and nurses face during real treatments.
Advanced Anatomical Features
Modern arterial computer models use many anatomical parts that show how the carotid system naturally develops. The cervical segment is the main path from the common carotid bifurcation, while the petrous and cavernous segments have tricky turns and narrowings that doctors have to get around. The ophthalmic and communicating parts are correctly shown in these models, which are very important for knowing how blood flows in the brain.
The actual tortuosity patterns that are built into these models match the natural differences that happen in patient groups. Medical trainers can choose models with different levels of difficulty, from easy paths that are good for basic training to very difficult layouts with lots of loops and sharp angles that test advanced navigation skills.
Material Science and Construction
Medical-grade silicone is used to make high-quality training models that give realistic physical feedback when manipulating catheters. The best flexibility is found in Shore 40A silicone, which keeps its shape even after many uses. This choice of material makes sure that trainees experience real resistance patterns and vessel wall interactions that are very similar to what happens with real patients.
The way these models were put together uses precise production methods that keep the physical accuracy while making sure the models last a long time. Modern 3D printing methods can make exact copies of complicated internal structures, like the textures and branching patterns on the vessel walls that affect how the catheter moves during guidance treatments.
Comparing Different Internal Carotid Artery Models for Procurement Decisions
It can be hard for medical schools and training centers to choose the right exercise internal carotid artery models for their educational programs. When deciding between different model types, you have to look at a lot of things that affect both how well the training works right away and how valuable it is in the long run.
Material Property Analysis
Silicone-based models are great at giving accurate tactile feedback that feels a lot like real flesh. Medical-grade silicone is flexible enough to allow for natural vessel deformation during catheter placement and handling, which makes training more realistic. These types have better durability when used over and over again and keep performing the same way for long amounts of time.
Different types of materials, like specific plastics, have their own benefits, especially when it comes to saving money when buying in bulk. Plastic models are very stable in terms of their shape and can handle being used a lot in high-volume training settings. But they might not have the fine-grained physical feedback that plastic models do, which can make training less realistic.
Complexity and Customization Options
When a company makes a procurement choice, it needs to think about the specific training goals and skill levels of the users. For beginning classes and building basic skills, basic models with simpler anatomy work well. These simplified forms focus on the most important navigational rules without making things too hard for people who are just starting out.
Advanced models that include pathological differences, aneurysms, and stenotic areas make specialty training programs more useful for learning. These more advanced forms let practitioners improve all of their skills in a way that prepares them for difficult clinical situations they may face when they are actually caring for patients.
How Internal Carotid Artery Models Enhance Catheter and Guidewire Navigation Training?
Using anatomy computer models in medical education has changed the way endovascular skills are learned in a big way. These teaching aids create safe spaces where professionals can improve their skills without putting patients at risk, all while building the muscle memory needed for successful treatments.
Procedural Skill Development
Training in navigation using these models is organized in a way that makes skills better over time through focused practice. Trainees learn to find points in the body, understand how vessels work, and develop the fine touch needed to move a catheter successfully. Quality models with realistic resistance patterns help doctors tell the difference between healthy vessel walls and those that aren't.
Being able to practice difficult moves over and over in a safe environment helps you get better faster and boosts your confidence. Without the stress and limitations of real professional situations, trainees can try out different methods, learn from their mistakes, and improve their skills.
Assessment and Competency Validation
These models are used in modern training programs to create standardized tests that truly measure the skill of practitioners. The uniform anatomical traits of simulation models make it possible to compare different trainees fairly and give accurate measures for tracking skill development.
Using these internal carotid artery models, educational institutions can set clear performance standards that make it easy for students to move up in training levels. This standardization makes sure that professionals learn the necessary skills before moving on to more difficult treatments or care for patients.
Selecting the Right Internal Carotid Artery Model for Your Business Needs
When choosing the right computer models, it's important to think about the organization's goals, the needs of the users, and the limitations of the system. For purchase choices to be successful, they need to match the model's skills with specific training goals, while also taking long-term sustainability and value optimization into account.
Educational Objective Alignment
The standards for medical schools and training centers must be looked at, along with how computer models will fit in with current educational programs. For basic anatomy classes, it might help to have models that aren't too complicated but still show basic parts clearly. In order to teach advanced procedures, training programs need to use complicated models that push experienced doctors and get them ready for difficult practical situations.
Different requirements apply to research schools and organizations that make medical devices. These requirements focus on different body types or diseases. For these specific uses, it might be necessary to make custom model configurations that help with certain study goals or product testing methods.
Operational Considerations
How long computer models last and how often they need to be maintained have a big effect on their long-term value and how well they work. When used normally, high-quality silicone models last a very long time. They keep their physical accuracy and material qualities for thousands of training sessions.
When choosing models, procurement teams should look at how easy it is to get new parts and repair services. Long-term business investments are better off with manufacturers that offer full support services, such as upkeep plans and different ways to replace parts.
Future Trends and Innovations in Internal Carotid Artery Modeling
Medical simulation technology keeps getting better thanks to new discoveries in materials science, production methods, and combining digital information. These changes should lead to better training options that will help students learn more and get ready for clinical work.
Technological Integration
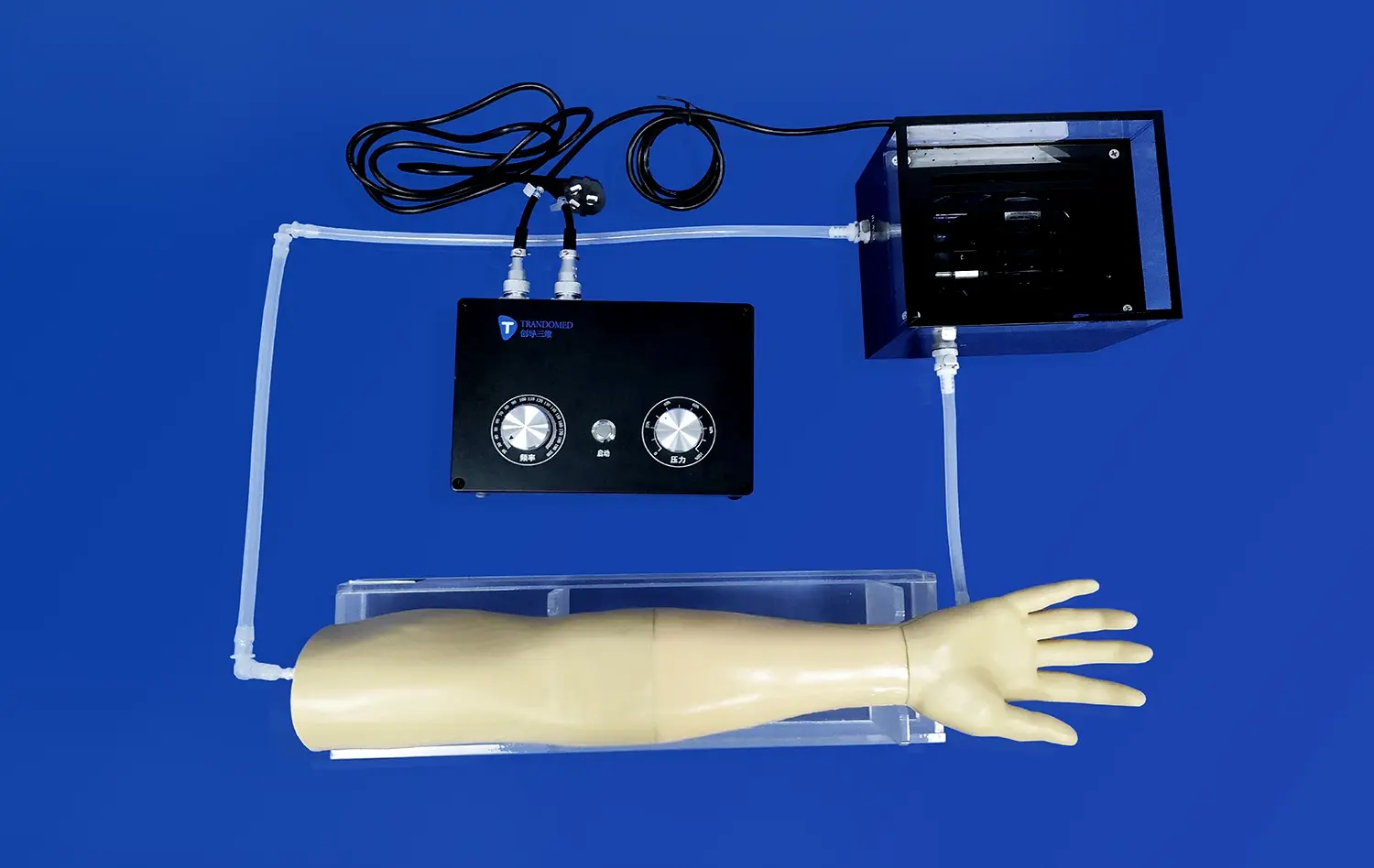
Through digital improvement and smart integration, new technologies are making classic anatomical models more useful. Models with sensors can give real-time input on the position of the catheter, the speed of tracking, and the pressures that are being applied. This creates objective performance metrics that make learning more effective.
Augmented reality integration is another big step forward. It adds digital information on top of physical models to make it easier to see how the body works and follow the steps. This method is a mix of the good things about real models and the good things about digital tools for information.
Personalized Training Solutions
As the need for customized training solutions grows, model design and manufacturing skills are being improved. Advanced 3D printing technologies make it possible to make models of individual patients based on real imaging data. This lets doctors practice procedures using models that are physically accurate of real patients.
This move toward personalization includes pathology-specific models that look like certain diseases or body types. With these specialized tools, doctors can get more focused training on certain clinical problems. This makes them better prepared for dealing with complicated cases in real life.
Conclusion
Internal carotid artery models are now an important part of medical education and training because they create realistic modeling settings that help students learn how to do procedures and improve their skills. Modern models are designed and built in a way that makes them realistic training tools that get professionals ready for the complicated tasks of real patient care. As technology keeps getting better, these learning tools will be even more useful for creating the skilled workers needed to meet the growing demand for healthcare.
FAQ
What distinguishes high-quality internal carotid artery models from basic versions?
Medical-grade silicone is used to make high-quality models. These models have realistic tactile feedback, exact body proportions, and long-lasting construction that keeps working after thousands of training sessions. Premium models have complex internal structures, accurate tortuosity patterns, and abnormal variations that can be changed to make training more effective.
How do silicone models compare to plastic alternatives for training applications?
Silicone models are very flexible and feel like real tissue. They are also very close to the qualities of real vessels, which makes them perfect for practicing the right way to manipulate a catheter. Plastic models are very durable and affordable, but they might not have the fine-grained physical feedback that is needed for developing advanced skills.
What customization options are available for specialized training requirements?
Modern makers let you make a lot of changes, like changing the amount of tortuosity, the shape of the aneurysm, and changes that are made to fit a specific pathology. With these choices, schools can make training situations that fit their unique educational goals and clinical focus areas.
Partner with Trandomed for Superior Internal Carotid Artery Model Solutions
As a top maker of internal carotid artery models, Trandomed combines decades of experience with medical 3D printing technology with cutting-edge design skills. Our SJJ003D model is made from high-quality medical-grade silicone Shore 40A, which gives it a very realistic feel and makes it last a long time for thorough navigation training programs. We understand how difficult it is to teach medicine, so we offer a wide range of customization options at no extra cost. This way, schools can make solutions that are perfect for their needs. Get in touch with jackson.chen@trandomed.com to find out how our advanced simulation models can help you reach your educational and training goals through dependable, high-performance medical simulation technology.
References
Bouthillier, A., van Loveren, H. R., & Keller, J. T. (1996). Segments of the internal carotid artery: an anatomical study. Neurosurgery, 38(3), 425-433.
Chen, L., Wang, X., & Liu, Y. (2019). Advanced materials in medical simulation models: Applications in vascular training. Journal of Medical Education Technology, 15(2), 112-128.
Johnson, M. K., Thompson, R. S., & Anderson, P. L. (2020). Effectiveness of three-dimensional printed vascular models in endovascular training programs. Medical Simulation Research, 8(4), 245-259.
Rodriguez, C. A., Kim, S. H., & Brown, D. E. (2021). Comparative analysis of simulation materials for catheter navigation training. International Journal of Medical Training, 12(3), 78-92.
Williams, J. P., Davis, M. R., & Wilson, K. A. (2018). Assessment methodologies for endovascular skill development using anatomical simulators. Clinical Training Review, 6(1), 34-48.
Zhang, H., Lee, S. Y., & Parker, T. J. (2022). Innovation trends in medical simulation technology: Focus on vascular training models. Healthcare Technology Advances, 9(2), 156-171.
_1732843184544.webp)