Mastering PICC line placement requires precision, skill, and extensive practice to ensure patient safety and optimal clinical outcomes. The realistic PICC model changes the way doctors are trained by giving them a realistic way to practice their skills by simulating the whole human vein system, from the arm to the superior vena cava. This advanced training tool bridges the important gap between theoretical knowledge and actual skill. It gives healthcare workers the chance to practice putting in catheters safely by using lifelike body parts and giving them feedback through touch.
Understanding the Challenges of PICC Line Placement
PICC line placement represents one of the hardest things that doctors have to do because they have to be very precise and know a lot about how blood vessels work. Healthcare workers often run into problems because they don't have enough training chances or because of the problems with standard ways of teaching.
Common Procedural Complications and Training Gaps
Because peripherally placed central catheter techniques are so complicated, there are many places where something could go wrong. A lot of the time, it's hard for clinicians to get the catheter in the right place, especially when they have to move from peripheral to central venous circulation. Traditional anatomical models don't give practitioners accurate physical feedback, so they aren't ready for the subtle differences in resistance and body structure that they will find during real treatments.
Procedure problems like misalignment, infection, and clotting are often caused by inadequate teaching methods. Healthcare workers can't build the muscle memory and spatial awareness they need to place catheters correctly because they don't have access to accurate simulation environments. These problems with training have a direct effect on the safety of patients and the success rates of procedures across all medical schools.
The Critical Need for Advanced Training Solutions
Today's healthcare needs teaching methods that help people go from knowing things in a theoretical way to using them in real life. For successful PICC line training, anatomy accuracy includes more than just being able to see the vein. It also includes being able to accurately perceive depth and feel the tissue. More and more healthcare organizations are realizing that engaging in advanced simulation technology leads to better patient results and fewer problems during procedures.
Introducing the Realistic PICC Model: Innovation in Training and Procurement
Traditional ways of training healthcare workers have never been able to prepare them for how hard it is to put in a PICC line in real life. Trandomed's revolutionary PICC model (XXS007) changes the way medical students learn by showing anatomy and functions in a way that has never been seen before.
Advanced Anatomical Design and Material Engineering
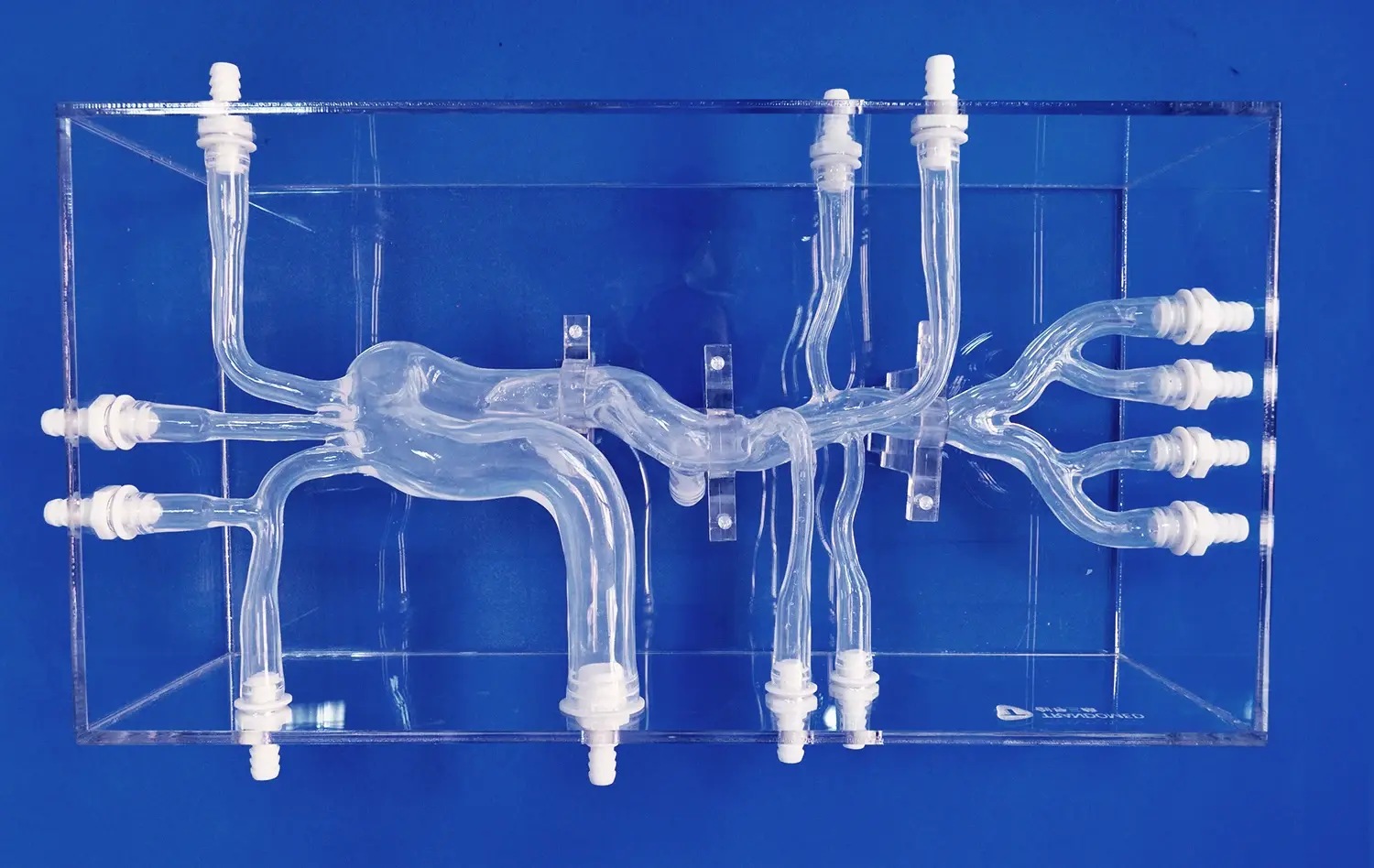
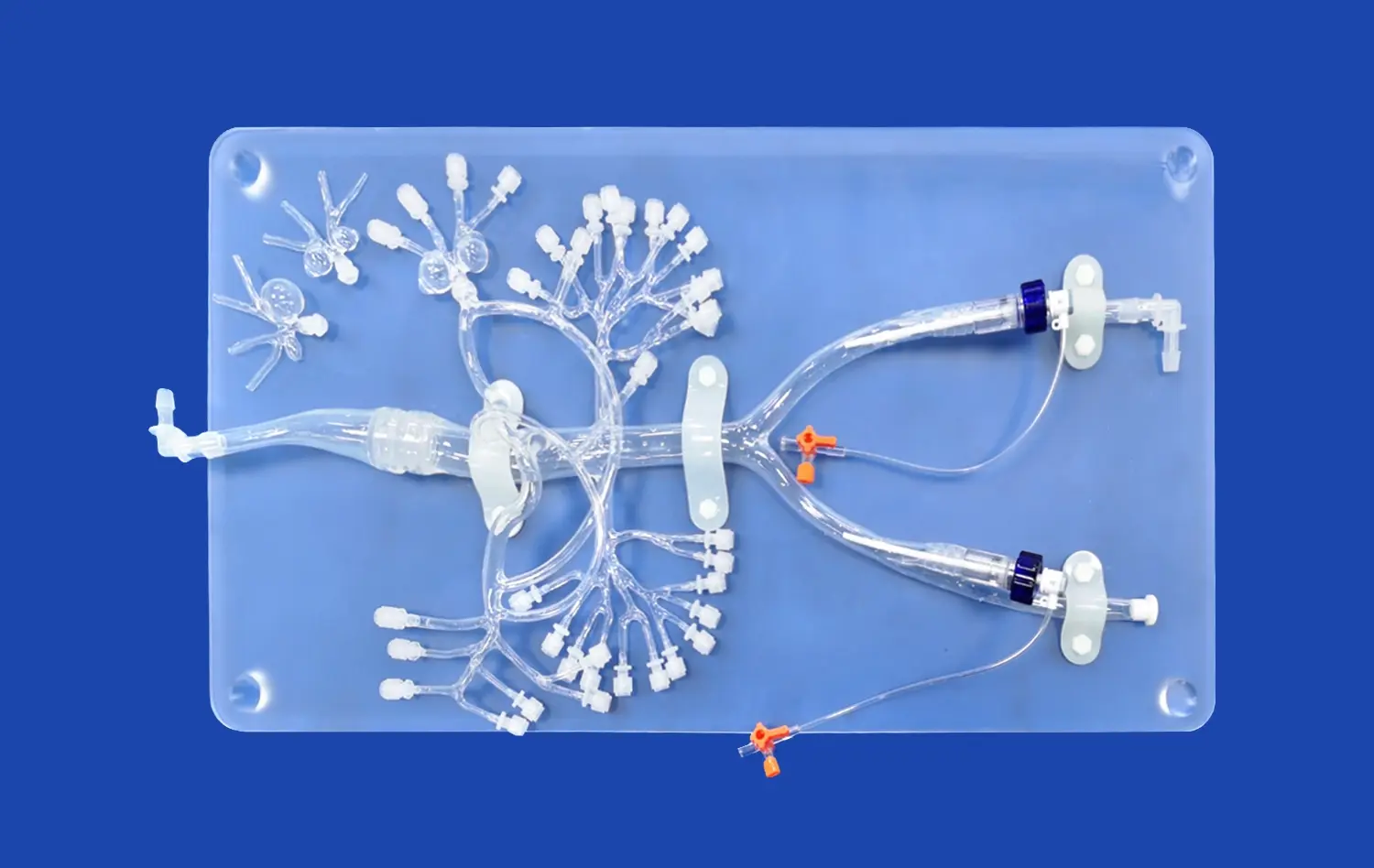
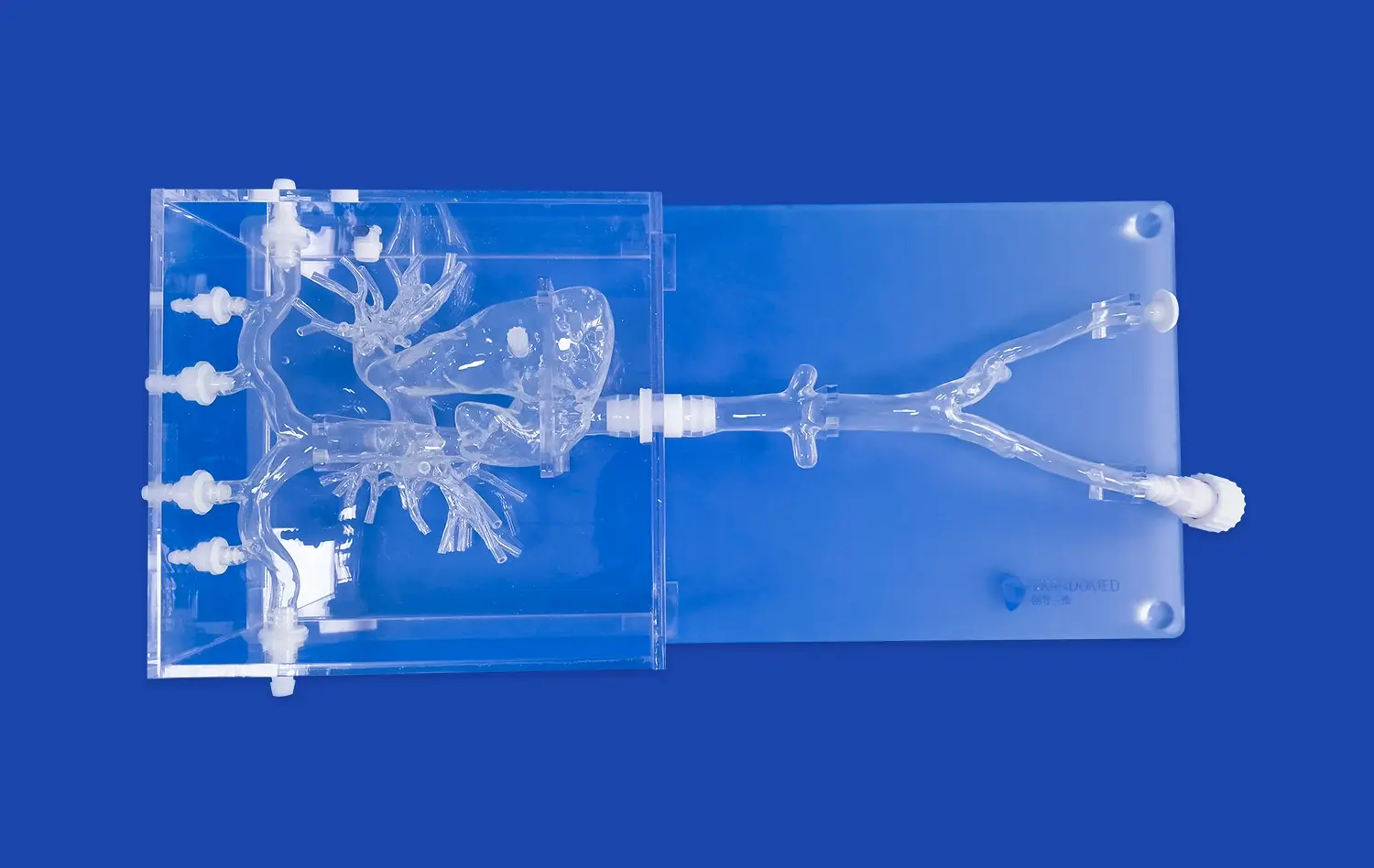
There are many types of veins in the XXS007 PICC training model. These include the brachial, basilic, cephalic, axillary, subclavian, brachiocephalic, internal and external jugular veins, superior and inferior vena cava, and right atrial structures. This model is made from high-quality Silicone Shore 40A material and gives real physical feedback that feels a lot like human tissue during catheter insertion processes.
Through the clear plastic shell, trainees can see the whole venous network from all sides, which helps them understand how different body parts are connectFed in space. Puncture valves strategically placed at the basilic, cephalic, brachial, and middle cubital veins allow for realistic puncture treatments while keeping the model's integrity through multiple training sessions.
Ultrasound Compatibility and Clinical Integration
Ultrasound guiding is becoming more and more important in modern PICC placement methods to get the best results. The realistic training model works with all ultrasound systems, so doctors can get better at using image-guided methods for placing catheters. This integration makes sure that training situations match up with the latest healthcare guidelines and best practices.
The model's design makes it possible to get full training in a number of different injection methods, so it can be used in a variety of clinical settings and follow different institutional standards. Healthcare workers can use the same training platform to practice both landmark-based and ultrasound-guided methods, which increases the value of the training and the number of ways it can be used.
Evaluating Core Steps for Optimal PICC model Line Placement Using the Model
To successfully place a PICC line, you need to follow a set of steps and pay close attention to every little detail. The advanced training program helps you improve all of your skills by giving you practice situations that are like real-life clinical settings.
Preparation and Setup Protocols
For training to work, the models and tools must be set up correctly. The PICC model works with normal clinical setting steps, such as preparing a sterile field, placing the ultrasound probe, and choosing a catheter. Trainees learn important steps that need to be taken before a procedure can begin. They also get used to using tools and organizing their area.
The model works with different kinds of catheters and guidewires, so it can be used with equipment that is preferred by the school. This adaptability makes sure that training is useful in a wide range of healthcare situations while still following standard procedures and safety rules.
Stepwise Insertion Techniques and Troubleshooting
The teaching platform provides full procedural education, from finding the first vessel to making sure the catheter is in the right place at the end. Trainees work on important skills like:
• Vessel identification and assessment: learning how to recognize venous anatomy and choose the best place to put the catheter using ultrasound help and palpation
• Sterile technique maintenance: following the right aseptic methods while placing the catheter, as well as keeping the tools and sterile fields clean.
• Catheter advancement and positioning: learning how to move the catheter safely through the veins while noting normal resistance patterns and anatomical landmarks
These in-depth training chances make sure that healthcare workers learn how to do procedures with confidence and that they know what problems could happen and how to fix them. Because the model gives accurate feedback, it is possible to see how the catheter should be placed and spot mistakes in placement before they happen in real life.
Advanced Complication Management Training
The modeling tool makes it easier to learn how to spot complications and deal with them. In a controlled learning setting, practitioners can experience situations where the catheter is in the wrong place, there is pushback during advancement, and other problems that can happen during the procedure. This training improves the ability to make professional decisions and the trust in how to do things when caring for real patients.
Procurement and Application: How to Choose and Use the Realistic PICC Model
Healthcare organizations and medical education facilities need to buy simulation tools in a way that balances quality, usefulness, and long-term value. As part of the decision process, the product's powers, the vendor's dependability, and the needs of institutional integration must all be carefully looked at.
Evaluation Framework for Medical Simulation Equipment
When choosing training simulations, procurement workers have to look at a number of factors, such as how accurate the models are of the body, how long the materials will last, and how well they teach. The XXS007 PICC training model performs better on these important measures thanks to improved manufacturing methods and quality control procedures.
Key evaluation factors include how long the model lasts when used over and over, how well it works with current training infrastructure, and how well the vendor can support the model. These needs are met by Trandomed's all-around service approach, which includes thorough quality testing, personalization choices, and ongoing technical support services.
Streamlined Purchasing and Implementation Process
The PICC model's buying process puts an emphasis on efficiency and customer happiness through good logistics and clear communication. Lead times of 7–10 days are normal, which allows for quick launch while still meeting quality standards. FedEx, DHL, EMS, UPS, and TNT are just a few of the shipping choices that can be used to meet the needs of customers in different areas.
Utilizing T/T plans for payment processing makes foreign transfers easier and more secure. The complete customization service lets schools make changes to designs without charging extra, so they can fit training tools to specific clinical and educational protocols.
Long-term Value and Support Considerations
Before buying high-tech medical training equipment, you should think about how it will help your business in the long run and how well the seller can support it. Trandomed's dedication to customer happiness goes beyond just delivering the goods. They offer extensive service and technical help programs after the sale as well.
Customers can be sure that the company's products will work and be reliable because they have a lot of experience with medical 3D printing technology and have a good track record with making simulators. Ongoing support services make sure that training stays useful and equipment lasts as long as possible, which helps healthcare institutions get the most out of their investments.
Conclusion
The realistic PICC model is a huge step forward in medical modeling technology. It fills in important training holes and improves both procedural trust and patient safety. This training platform helps healthcare workers learn how to properly place catheters in controlled learning settings by having physically correct designs, high-quality materials, and a lot of features. When realistic tactile feedback, ultrasound compatibility, and structured procedural training come together, they make a tool that medical schools that want to provide the best clinical education and patient care can't do without.
FAQ
What is a peripherally inserted central catheter used for?
A PICC line gives doctors safe access to large veins near the heart, which lets them safely give medicines and treatments that might otherwise hurt smaller vessels in the body's edges. This special tube can be used for many medical purposes, such as giving chemotherapy, parenteral feeding, antibiotics, and other medicines that need to go into a central vein. Because there is more blood in central veins, medications can be diluted quickly. This lowers the risk of vessel soreness and gets rid of the need to place needles over and over again during long treatment plans.
What is the purpose of using a peripherally inserted central venous catheter?
Doctors suggest PICC lines when treatment plans need to access a vein often for long periods of time, usually a few weeks to a few months. Cancer treatments involving chemotherapy and targeted therapy drugs work better with PICC line delivery because there is less chance of damaging nearby blood vessels. PICC lines are used to give vital nutrients to patients who need total parenteral nutrition because of problems with their digestive systems. PICC lines are also used for dangerous diseases that need long-term antibiotic or antifungal treatment to make sure that the right medicine is given safely and to keep the patient from feeling too much pain from having needles put in over and over again.
How long can a PICC line stay in?
PICC lines can stay in place safely for a few months as long as they are taken care of and checked for any problems. It is held in place with special clips and kept safe with clear plastic coverings that let you see what's going on while keeping things clean. This long-term accessibility gets rid of the need for multiple needle insertions during chemotherapy cycles or long medication regimens. This makes patients much more comfortable and helps them stick with their treatment, while also lowering the stress of the procedure for both patients and healthcare workers.
What problems may occur with PICC catheters?
Some problems that can happen with a PICC line are getting an infection at the insertion site or along the catheter tube, the catheter getting blocked by blood clots or drug precipitates, thrombosis forming in nearby blood vessels, and very rarely, the catheter breaking or splitting. These problems show how important it is to use the right insertion method, follow regular upkeep instructions, and keep an eye out for signs of failure. As part of their comprehensive training, healthcare workers learn how to avoid issues and know what to do when problems do happen through realistic exercise models.
Elevate Your Medical Training with Trandomed's Advanced PICC Model Solutions
Trandomed changes the way medical education is done by using cutting edge 3D printed modeling technology that makes practical training more effective. Healthcare workers can confidently learn how to place a catheter with our XXS007 PICC model, which has the most accurate anatomy and most realistic procedure experience. Trandomed is China's top PICC model maker, with more than 20 years of experience in medical 3D printing innovation. They offer options that can be changed to fit the needs of your school. Get in touch with jackson.chen@trandomed.com to find out how our cutting-edge modeling tools can help your training programs and make things better for your patients.
References
Chopra, V., Flanders, S. A., Saint, S., & Woller, S. C. (2012). The Michigan Appropriateness Guide for Intravenous Catheters (MAGIC): Results from a multispecialty panel using the RAND/UCLA appropriateness method. Annals of Internal Medicine, 163(6), S1-S40.
Gorski, L., Hadaway, L., Hagle, M. E., McGoldrick, M., Orr, M., & Doellman, D. (2016). Infusion therapy standards of practice. Journal of Infusion Nursing, 39(1S), S1-S159.
Schiffer, C. A., Mangu, P. B., Wade, J. C., Camp-Sorrell, D., Cope, D. G., El-Rayes, B. F., & Brouwers, M. C. (2013). Central venous catheter care for the patient with cancer: American Society of Clinical Oncology clinical practice guideline. Journal of Clinical Oncology, 31(10), 1357-1370.
Moureau, N., Poole, S., Murdock, M. A., Gray, S. M., & Semba, C. P. (2002). Central venous catheters in home infusion care: outcomes analysis in 50,470 patients. Journal of Vascular and Interventional Radiology, 13(10), 1009-1016.
Alexandrou, E., Ray-Barruel, G., Carr, P. J., Frost, S. A., Inwood, S., Higgins, N., & Rickard, C. M. (2018). Use of short peripheral intravenous catheters: characteristics, management, and outcomes worldwide. Journal of Hospital Medicine, 13(5), 303-312.
Brass, P., Hellmich, M., Kolodziej, L., Schick, G., & Smith, A. F. (2015). Ultrasound guidance versus anatomical landmarks for subclavian or femoral vein catheterization. Cochrane Database of Systematic Reviews, 1, CD011447.

_1734504197376.webp)