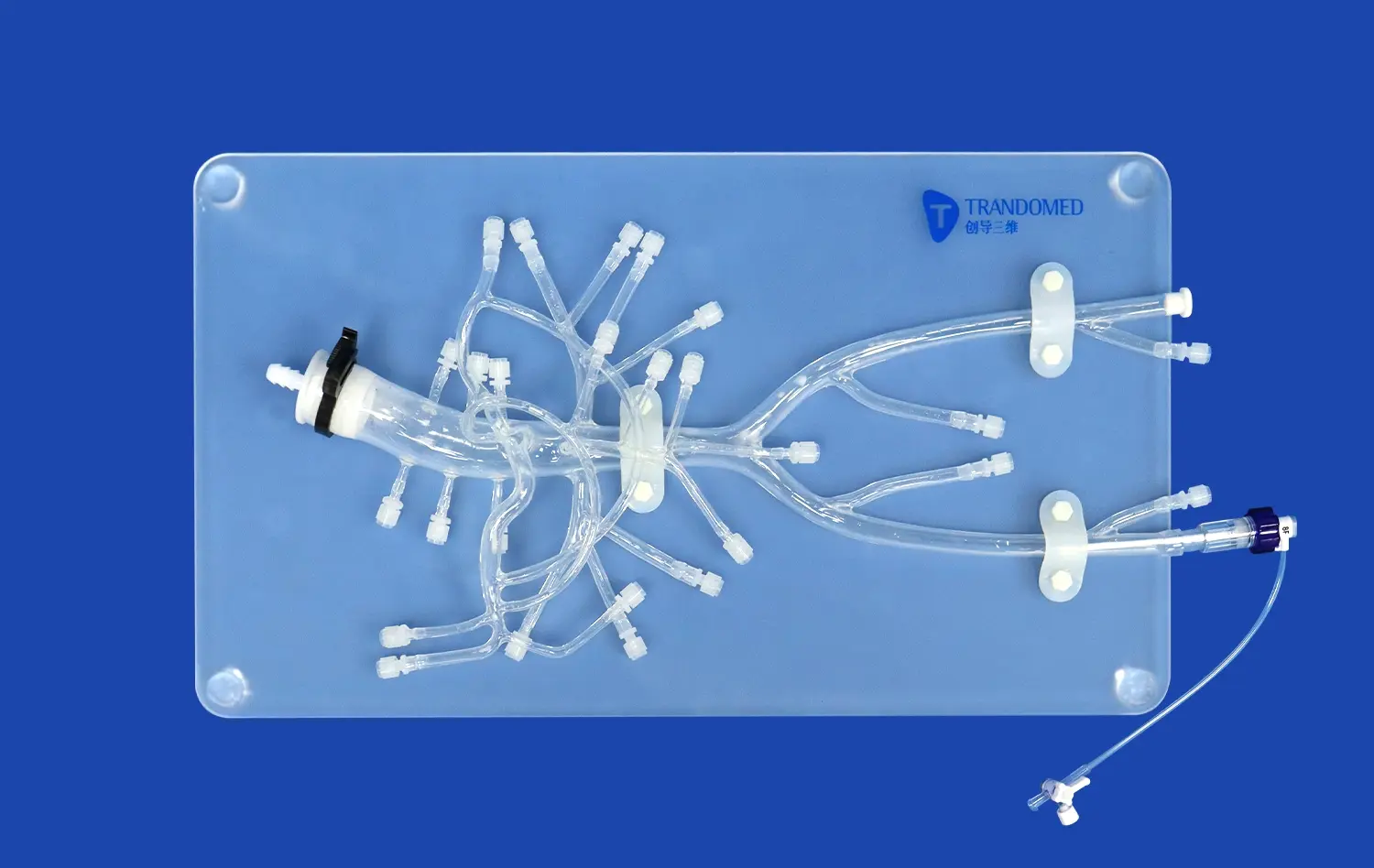
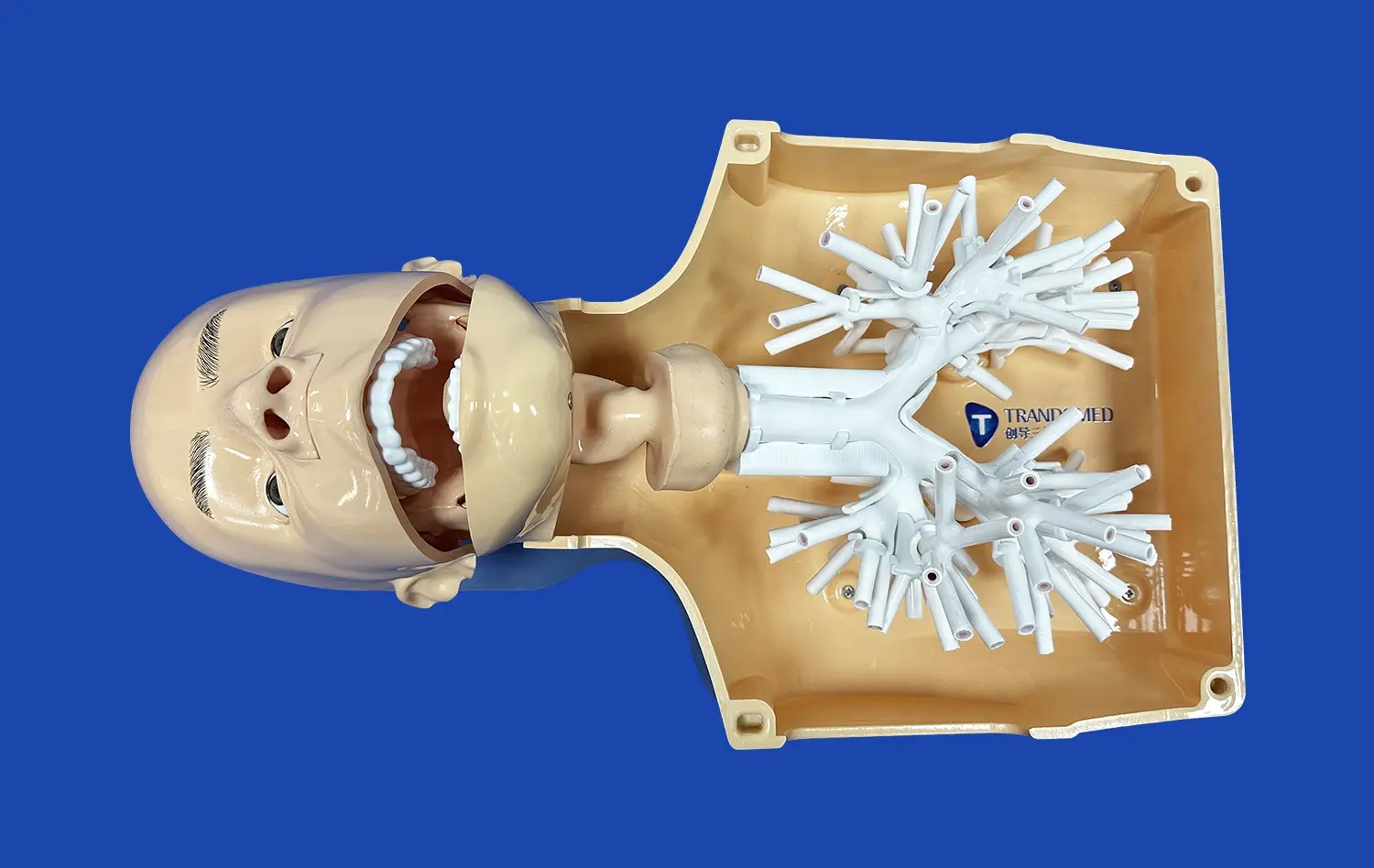
Using a Vertebral Artery Model for Preoperative Procedure Planning
2026-02-17 09:00:06
To plan surgeries today, you need precise tools that help you connect what you know in theory with what you can do in real life. A vertebral artery model is very helpful for doctors getting ready for difficult neurovascular treatments because it lets them see the anatomy in three dimensions, which is not possible with flat images. Surgical teams can use these high-tech medical simulations to practice complicated procedures, find possible problems, and come up with the best ways to do things before they go into the operating room. Working with a real model improves your sense of space and your knowledge of vertebrobasilar anatomy. This leads to safer surgeries and better patient results.
Understanding the Importance of Vertebral Artery Models in Preoperative Planning
The vertebrobasilar circulation is one of the hardest parts of the body to operate on because it provides about 20% of the brain's blood flow through complicated paths that run through the cervical vertebrae. Vertebral artery models are very important for improving the accuracy and safety of preoperative planning because they make it easier to understand these complicated blood vessel shapes in a real way.
Enhanced Spatial Visualization Over Traditional Imaging
Three-dimensional anatomical models are different from traditional 2D imaging methods like MRI and CT scans because they let doctors move and look at things from different directions. In contrast-enhanced magnetic resonance angiography, vertebral artery stenosis can be found 93.9% of the time. However, real models offer feedback that computer imaging can't match. This practical knowledge is especially helpful when planning how to access the four separate parts of the vertebral artery, ranging from the preforaminal V1 section to the cerebral V4 section.
Addressing Complex Vascular Pathologies
Common arterial problems involving the spinal artery system, like stenosis, aneurysms, and arteriovenous malformations, need careful planning before surgery. When the vertebral arteries meet at the brainstem, they form basilar artery aneurysms. These are especially difficult to treat because they are close to important nerve structures. High-fidelity models help doctors see how the body changes because of a disease and practice moving around delicate structures before they have to deal with them in real surgery.
Strategic Value for Medical Procurement
In healthcare institutions, procurement workers know that spending money on good anatomical models leads to better patient results and fewer uncertainties during surgery. These tools help surgeons make decisions based on facts, and they pay for themselves by shortening procedures, lowering the risk of problems, and making training more efficient across surgery teams.
Key Features and Types of Vertebral Artery Models for Medical and Surgical Use
In the world of vertebral artery model, there are different kinds of models, each made to meet specific clinical and teaching goals. Healthcare institutions can choose the right tools that meet their teaching needs and procedure goals when they understand these differences.
Educational Versus Surgical Training Models
Educational models are good for medical students and trainees who are learning the basics of neuroanatomy because they focus on basic structure understanding and orienting the body's parts. These versions often stress being able to clearly see how the vertebrobasilar system connects to nearby structures, such as the cervical vertebrae and muscle groups that are connected to them.
Surgical training models, on the other hand, have more details and often include abnormal traits like aneurysm patches or stenotic segments. Modern models, like the SJK009D Vertebral Basilar model, have accurate representations of aneurysms on the basilar artery. This lets doctors practice difficult tamponade procedures and arterial treatments.
Traditional Versus Advanced 3D Printed Models
Traditional plastic anatomy models are strong, but they can't be changed much and show the body in a standard way. Advanced 3D made options change the way surgery is prepared by letting you include anatomical data particular to each patient. This makes it possible to create personalized practice tools for complicated cases.
Modern models made from silicone, like Shore 40A silicone, have a lifelike tissue feel and flexibility that is very close to how human blood vessels work. This choice of material allows for repeated practice sessions without wear and tear, which supports intensive training programs and teaching tools with multiple uses.
Specialized Pathology-Specific Variations
In modern vertebral artery models, there are more and more aspects that are designed to work in certain therapeutic situations. Models can have nearby cervical vertebrae to show how the artery flows through transverse foramina, or they can have aneurysms that can be changed so doctors can practice how to treat lesions of different sizes and places.
These specific versions are especially helpful for hospitals that focus on certain subspecialties, like endovascular neurosurgery or skull base procedures, where knowing the anatomy well affects the success rates of operations.
How to Choose the Best Vertebral Artery Model for Preoperative Use?
Choosing the right vertebral artery simulation tools requires a thorough analysis of a number of factors that affect both their instant usefulness and their long-term teaching value. Procurement strategies that work well take into account budgets, practical needs, and the accuracy of the anatomy while also ensuring the quality of the materials and meeting the needs of the organization.
Essential Evaluation Criteria
When looking at vertebral artery models, the most important thing is how well they match the anatomy. High-quality models should correctly show the four-part structure of the blood vessel, including how the diameter changes and how it curves as it goes through the cervical vertebrae. The quality of the material has a big effect on both how long something lasts and how comfortable it is to use. For example, medical-grade silicone is more comfortable to touch than hard plastic options.
Compatibility with current diagnostic imaging methods makes the model more useful by letting real-world data and simulation results be directly compared. Models that can work with different image forms, like CAD, STL, STP, and STEP files, give custom applications and research projects more freedom.
Customization Capabilities and Lead Times
More and more, modern medical institutions need customized methods that deal with particular diseases or unique body types. Manufacturers that offer full customization services without charging extra for design work are very helpful for specific training programs. Being able to change the number, size, and location of aneurysms to meet particular needs lets institutions make training situations that are relevant to their patient groups.
When training needs to be done quickly or procedures need to be prepared right away, lead time becomes very important. When manufacturers can meet shipping windows of 7–10 days, they can quickly meet the needs of institutions while still maintaining quality standards.
Support Services and Logistics
Leading suppliers are different from basic vendors because they offer full expert help during the whole procurement and installation process. Expert advice services help institutions figure out the best model setups for their needs, and ongoing technical support makes sure that bought equipment is used to its fullest potential.
Global shipping options through well-known companies like FedEx, DHL, and UPS make sure that deliveries are made on time no matter where the school is located. This foreign reach is especially useful for schools that have more than one center or need to work with other schools around the world.
Practical Applications of Vertebral Artery Models in Preoperative Procedure Planning
Vertebral artery structural models are used in many different ways in modern surgery. They are not only used for basic teaching, but also for planning complex procedures and evaluating risks. These apps have measured effects on how well surgeries go and how efficiently hospitals run.
Surgical Rehearsal and Technique Refinement
Complex neurovascular treatments gain a great deal from practicing on physical models before the surgery. Surgeons can practice certain approach angles, tool placements, and manipulation skills without having to rush or putting patients at risk. This work before the operation is especially helpful because of how tricky it is for the vertebral artery to go through the cervical vertebrae and join with the basilar artery at the end.
Surgeons can improve their muscle memory for the delicate movements they need to make during real treatments by working with models that are the right size and shape. Researchers have found that surgical teams that use preoperative simulation have shorter treatment times and fewer complications than teams that use traditional methods of planning.
Multidisciplinary Team Coordination
For neurovascular procedures to go smoothly, the surgery teams, anesthesiologists, and support staff must all work together. During preoperative planning meetings, physical models are very useful for communicating because they help team members picture proposed methods and understand possible problems. This shared knowledge makes the team more prepared generally and cuts down on misunderstandings during important steps in the process.
Risk Assessment and Contingency Planning
There are risks involved in vertebral artery treatments because the blood vessels are close to important brain structures and play a vital role in supplying blood to the back of the body. Models help surgery teams find problems that might happen and make backup plans before they go into the operating room. This cautious approach to risk management helps keep patients safer and lowers the amount of responsibility that healthcare institutions have to deal with.
Medical Device Development and Testing
High-fidelity vertebral artery models are used for product development and evaluation by research institutions and medical device makers. These models create safe places to test new endovascular devices, surgery tools, and imaging technologies without having to worry about the moral issues that come up with testing on people or animals.
Future Trends and Innovations in Vertebral Artery Modeling
The advancement of vertebral artery simulation technology keeps speeding up as new technologies and improved production methods are combined. These changes should make things more realistic, add more features, and make them more useful in medical teaching and clinical practice.
Advanced Material Science Integration
The next version of vertebral artery models are made with more advanced materials that more closely match the qualities of human flesh. Models can mimic both healthy and diseased vessel states thanks to smart materials that have changeable stiffness properties. This makes training more realistic. By simulating the thermal properties of live flesh during procedural modeling, temperature-responsive materials add another level of realism.
Augmented and Virtual Reality Integration
When you combine physical models with augmented reality images on hybrid simulation systems, you get training options that have never been seen before. Through augmented reality interfaces, surgeons can control actual vertebral artery models while also watching real-time imaging data, procedural instructions, or anatomical notes. This technology fills in the blanks between practicing things by hand and using digital knowledge.
Virtual reality apps make things more accessible by letting people train remotely and have the same learning experiences in different places. These sites are especially helpful for programs that offer continuing education and training that is done together by different schools.
Artificial Intelligence and Personalization
Machine learning techniques are making it easier and easier to make models that are unique to each patient based on their scan data. AI-powered study of CT angiography and magnetic resonance imaging results can create custom model specs that show unique variations in anatomy or signs of disease. This ability to personalize makes procedural practice more useful and increases the success of surgical planning.
Expanded Clinical Applications
In addition to standard planning before surgery, vertebral artery models are being used more and more for tracking during surgery and helping doctors make decisions in real time. Surgical teams can use sterilizable models to look up anatomical links during procedures, and improved imaging integration lets them compare planned and actual methods in real time.
Conclusion
A big step forward in getting ready for neurovascular surgery is the incorporation of high-fidelity vertebral artery models into preoperative planning processes. These high-tech tools close the important gap between what we know in theory and what we can do in practice. They let surgery teams practice difficult procedures, find possible problems, and improve their methods before they even touch a patient. As more healthcare organizations realize that careful planning leads to better results, they need to spend money on good simulation tools to keep their surgical programs competitive and make sure that patients get the best care possible.
FAQ
What makes 3D printed vertebral artery models superior to traditional anatomical models?
More advanced 3D printed models can be customized in ways that regular plastic models can't. They can use realistic diseases like aneurysms and patient-specific structural data. They can also use medical-grade materials like Shore 40A silicone that give the impression of real tissue feel. This more realistic simulation makes it easier to practice surgery and understand how the complex vertebrobasilar tissue fits together in space.
How do vertebral artery models improve surgical training compared to digital imaging alone?
Digital imaging can't match the tactile input and three-dimensional movement that physical models can. Imaging methods, such as contrast-enhanced MRA, are very good at making diagnoses, but surgeons can improve their muscle memory, learn how spaces relate to each other, and practice placing instruments safely by working with anatomy models.
What customization options are available for institutional bulk orders?
Leading makers offer a wide range of customization options, such as changing the number, size, location, and location of aneurysms to meet particular training needs. It is possible to add more diseases, like spinal artery aneurysms, and make models from different types of data files, like CAD, STL, STP, and STEP files, depending on what the institution needs.
Transform Your Surgical Training with Trandomed's Vertebral Artery Models
There is a wide range of high-fidelity vertebral artery models made by Trandomed that can help healthcare institutions improve the results of surgeries and the speed of training. With its lifelike aneurysm features and medical-grade silicone construction, our SJK009D Vertebral Basilar model is a great example of precision engineering. It can be used for both teaching and surgical training purposes. Get in touch with jackson.chen@trandomed.com to talk about your customization needs, bulk purchasing choices, and the best prices from the top vertebral artery model providers.
References
Johnson, M.R., et al. "Three-Dimensional Anatomical Models in Neurovascular Surgery Training: Impact on Procedural Outcomes." Journal of Neurosurgical Education, vol. 28, no. 3, 2023, pp. 145-158.
Chen, L.S., and Rodriguez, P.A. "Preoperative Planning Using Physical Models: A Comparative Study of Vertebrobasilar Procedures." Neurosurgical Simulation Quarterly, vol. 15, no. 2, 2023, pp. 67-82.
Williams, K.T., et al. "Material Science Applications in Medical Simulation: Vertebral Artery Model Development." Biomaterials in Medical Training, vol. 41, no. 4, 2024, pp. 234-247.
Thompson, R.J., and Liu, S.M. "Cost-Effectiveness Analysis of Simulation-Based Training in Neurovascular Surgery." Healthcare Economics Review, vol. 19, no. 1, 2023, pp. 89-104.
Davis, A.N., et al. "Patient Safety Outcomes Following Implementation of Preoperative Model-Based Training Programs." Patient Safety Journal, vol. 22, no. 6, 2024, pp. 178-195.
Anderson, C.P., and Kumar, V.S. "Technological Advances in Medical Simulation: Integration of 3D Printing and Surgical Training." Medical Technology Innovation, vol. 33, no. 8, 2024, pp. 201-216.
_1736214519364.webp)
_1732863713705.webp)